Today, Joe Landson shares his experience as a standard, real patient.
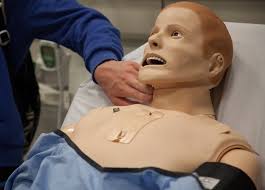 I work occasionally as a standardized patient, though there is not much standard about me.
I work occasionally as a standardized patient, though there is not much standard about me.
Standardized patients are actors; we play out a script of symptoms for health care providers and providers-in-training, to prepare them for real-life patients. It’s pick-up work. I do it one or two days per month, on average. And that minimal employment is fine for me, because in real life, I’m dealing with a debilitating disease that most doctors don’t think exists. I’m living with Myalgic Encephalomyelitis, better known as Chronic Fatigue Syndrome. I have no stamina left. All attempts to work full time, or even steadily part-time, have failed, and have usually left me bedridden. I rarely find myself able to put two good days together. Every day in which I feign functionality and sociability, I follow with (several) days of melting into a bed, couch, or easy chair. I’m reduced to a physical, mental, and emotional wreck, simply by acting normal.
In my acting work, I usually meet trainees trying to do a good job and make a good impression. In real life, I usually face doctors who have no idea what to do with me, and try to pawn me off on someone else. At work, I train; in real life, I face skeptical providers struggling with a disease for which no one has trained them.
In both worlds, you’re expected to check the boxes, however pointless this may seem. Once, I had a training session on how to deliver bad news to a grieving parent. I played the parent. The two doctors-to-be could not have been more different in their presentation. The first skipped several steps of his rubric in telling me my young son was not likely to make it out of the pediatric oncology ward. He even swapped my stage name with my ‘son’s’ name, which would obviously be awful in real life. Nonetheless, he succeeded in having a warm sympathetic tone combined with normal human language, and this made all the difference.
The second trainee checked all the boxes. He was clearly prepared to deliver bad news by the numbers, just as the script had taught him. Yet I didn’t enjoy this encounter as much. Why? He lacked a sympathetic tone. He seemed, at some points, to be serving a client on his way to shouting ‘Next!’.
Now, consider an actual medical encounter. The Veterans Affairs clinic has an intake form screening for suicidal thoughts and pain, amongst other things. Are you in any pain? Yes, my back hurts. Upper, middle, or lower back? Well, nurse, my entire spinal cord feels like it’s filled with mild acid, until I exert myself, when the acid slowly intensifies to excruciating levels. No, patient, that is not a valid answer. The pen hovered. Pick upper, middle, or lower. Next! I am not standard; I must learn to follow the script. I never do. I couldn’t play my role when the VA decided that ME/CFS sounded like Post-Traumatic Stress Disorder (PTSD), and treatment for that only annoyed me, or made me worse. As Dr. Nancy Klimas said in a March 2009 interview, if ME/CFS patients have PTSD, it’s from medical encounters.
One Monday, I scheduled an appointment (a real one) through my VA clinic, or rather took the date they gave me in the far distant future. The next day, my standardized patient manager asked me to work a gig… on the very same day of my VA appointment. It had finally happened. My fake medical life had stomped on my real medical life, and the joke is, both are fake. My life has gone full Franz Kafka. You’re welcome.
We managed to resolve the scheduling conflict, but obviously not the underlying one. The sum total of my medical interaction is a hoax, a lie, a simulation. Real or fake, all my medical ‘appointments’ reinforce that there’s not likely to be any effective care for me, because I’m not standard. Patients like me do not fit in today’s medicine. Psychiatry tries to claim us, but fails in shoddy efforts like the PACE Trial. Some doctors have explained to my face that the disease does not exist. It’s not the doctors’ fault, at least not entirely. While research exists, much is contradictory or unreliable. This makes it very hard even to diagnose ME/CFS, let alone to know what to do about it when it is.
Advances in immune science and medicine have lately shown a glimmer of hope in explaining ME/CFS, but we’re not at proof yet, let alone at effective treatment. So I guess I’ll keep living my fake life, until I finally become just as insane as some doctors already think I am.
I should mention, I can only do this occasional standardized patient gigs because my senior citizen mother drives me to and from them. If I drove myself, or took the noisy, floundering Metrorail train, I would tire out all the faster. Then again… I could always ride my coal bucket, just like Kafka in his story.
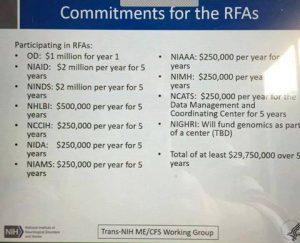








The Cut
Trump’s proposed budget is out. Among all the cuts – because you have to cut in order to increase defense spending while simultaneously giving the rich a tax cut – among all these cuts is one that people with ME should take very personally. NIH’s budget will be cut by 18% or $6 billion in fiscal year 2018, if Trump’s budgets passes as is. The proposed budget also calls for a reorganization of NIH’s Institutes, but offers little detail. Here’s how I feel about that:
https://twitter.com/infinite_scream/status/842728318910828548
Hang on. That wasn’t enough.
via GIPHY
Yeah, that’s how I feel.
This is nothing short of disastrous. NIH is the largest source of biomedical research in the world. NIH scientists discovered the bacteria that causes Lyme disease. They demonstrated the effectiveness of the first drugs used to treat AIDS. The biomedical research enterprise in the United States is built on NIH as its foundation. Cutting that foundation by 18% will be catastrophic for human health.
In addition, more than 80% of NIH’s budget goes out the door to fund academic biomedical research, largely in the United States. How will researchers do their research? I guess they’ll have to do 18% less of it. But it won’t just affect those researchers’ salaries paid by their grants, or the purchase of equipment (I wonder what will happen to the businesses that supply that equipment?), or the training of doctoral and post doctoral students. It will affect American universities, research hospitals, and other research institutions.
The university system is dependent on indirect costs tacked on to grants. Indirect costs are a percentage added to a grant by the university. It covers the costs associated with university infrastructure, like buildings and administration and libraries. If NIH’s budget is cut by 18%, then NIH will fund substantially less academic research. And if substantially less academic research is being funded, then American universities are stuck holding the bag. Because universities will still have buildings and staff and libraries, but a big chunk of that cost will not be covered by the indirect costs normally charged to grants. Trump’s budget may cut taxes for the rich, but it’s one hell of a tax on our universities.
This girl captures my response to this foolishness.
If the negative impacts of such a dramatic cut to NIH are that easy to identify, why is Trump proposing to do it? Apart from Trump’s desire to increase defense spending while cutting taxes, the Administration’s director of the White House Office of Management and Budget offered this explanation: “We think there’s been mission creep” at the NIH, he said. “We think they do things that are outside their core functions.”
Ok, but so what, right? After all, it’s not like NIH spends a whole lot on ME. Just $7.6 million in 2016. So who cares if NIH has a funding cut, right?
Are you prepared for an 18% reduction in ME spending?
I’m not. For one thing, the first year of funding for the new Collaborative Research Centers is set aside in this year’s budget. But all bets are off going forward. Like many other RFAs, the one for ME Centers explicitly states, “Future year amounts will depend on annual appropriations.” So it is possible that future years of funding could be cut or eliminated.
It’s common sense to conclude that if NIH’s budget is cut by 18% next year, every program and RFA and grant pool will be severely cut. NIH will make far fewer grants, and that will hit everybody hard.
But that could even be a best case scenario. After all, if I’m NIH and my choice is between an HIV/AIDS study and an ME study, there are a lot of reasons why I’m going pick HIV. Biodefense? Flu? Alzheimer’s Disease? Epilepsy? Spinal cord injury? Osteoporosis?
We’re not winning out against those diseases now. Do you really think that NIH will say, well, we should spread that 18% cut around evenly across the board. Do you expect that this cut will be applied fairly? Is any university going to support a faculty member who wants to apply for an ME grant instead of . . . basically any other disease?
ME research is stigmatized now. ME research is on a starvation diet now. What happens in any system when resources become more scarce? The weakest members of the system lose. And they lose hard.
Whatever your political views or affiliations, whatever you think of the current Administration, if you want to protect research funding then you have to make your voice heard. Call your Representative today. Make sure he/she knows that you support NIH funding and ask him/her to do the same.