Today, Joe Landson shares his experience as a standard, real patient.
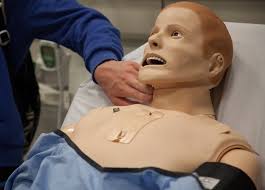 I work occasionally as a standardized patient, though there is not much standard about me.
I work occasionally as a standardized patient, though there is not much standard about me.
Standardized patients are actors; we play out a script of symptoms for health care providers and providers-in-training, to prepare them for real-life patients. It’s pick-up work. I do it one or two days per month, on average. And that minimal employment is fine for me, because in real life, I’m dealing with a debilitating disease that most doctors don’t think exists. I’m living with Myalgic Encephalomyelitis, better known as Chronic Fatigue Syndrome. I have no stamina left. All attempts to work full time, or even steadily part-time, have failed, and have usually left me bedridden. I rarely find myself able to put two good days together. Every day in which I feign functionality and sociability, I follow with (several) days of melting into a bed, couch, or easy chair. I’m reduced to a physical, mental, and emotional wreck, simply by acting normal.
In my acting work, I usually meet trainees trying to do a good job and make a good impression. In real life, I usually face doctors who have no idea what to do with me, and try to pawn me off on someone else. At work, I train; in real life, I face skeptical providers struggling with a disease for which no one has trained them.
In both worlds, you’re expected to check the boxes, however pointless this may seem. Once, I had a training session on how to deliver bad news to a grieving parent. I played the parent. The two doctors-to-be could not have been more different in their presentation. The first skipped several steps of his rubric in telling me my young son was not likely to make it out of the pediatric oncology ward. He even swapped my stage name with my ‘son’s’ name, which would obviously be awful in real life. Nonetheless, he succeeded in having a warm sympathetic tone combined with normal human language, and this made all the difference.
The second trainee checked all the boxes. He was clearly prepared to deliver bad news by the numbers, just as the script had taught him. Yet I didn’t enjoy this encounter as much. Why? He lacked a sympathetic tone. He seemed, at some points, to be serving a client on his way to shouting ‘Next!’.
Now, consider an actual medical encounter. The Veterans Affairs clinic has an intake form screening for suicidal thoughts and pain, amongst other things. Are you in any pain? Yes, my back hurts. Upper, middle, or lower back? Well, nurse, my entire spinal cord feels like it’s filled with mild acid, until I exert myself, when the acid slowly intensifies to excruciating levels. No, patient, that is not a valid answer. The pen hovered. Pick upper, middle, or lower. Next! I am not standard; I must learn to follow the script. I never do. I couldn’t play my role when the VA decided that ME/CFS sounded like Post-Traumatic Stress Disorder (PTSD), and treatment for that only annoyed me, or made me worse. As Dr. Nancy Klimas said in a March 2009 interview, if ME/CFS patients have PTSD, it’s from medical encounters.
One Monday, I scheduled an appointment (a real one) through my VA clinic, or rather took the date they gave me in the far distant future. The next day, my standardized patient manager asked me to work a gig… on the very same day of my VA appointment. It had finally happened. My fake medical life had stomped on my real medical life, and the joke is, both are fake. My life has gone full Franz Kafka. You’re welcome.
We managed to resolve the scheduling conflict, but obviously not the underlying one. The sum total of my medical interaction is a hoax, a lie, a simulation. Real or fake, all my medical ‘appointments’ reinforce that there’s not likely to be any effective care for me, because I’m not standard. Patients like me do not fit in today’s medicine. Psychiatry tries to claim us, but fails in shoddy efforts like the PACE Trial. Some doctors have explained to my face that the disease does not exist. It’s not the doctors’ fault, at least not entirely. While research exists, much is contradictory or unreliable. This makes it very hard even to diagnose ME/CFS, let alone to know what to do about it when it is.
Advances in immune science and medicine have lately shown a glimmer of hope in explaining ME/CFS, but we’re not at proof yet, let alone at effective treatment. So I guess I’ll keep living my fake life, until I finally become just as insane as some doctors already think I am.
I should mention, I can only do this occasional standardized patient gigs because my senior citizen mother drives me to and from them. If I drove myself, or took the noisy, floundering Metrorail train, I would tire out all the faster. Then again… I could always ride my coal bucket, just like Kafka in his story.

I hope this reaches far and wide to help the rest of the world begin to understand that many of us only have one or two days of month when we can feign normalcy.
Thank you Joe!
You’re welcome, Denise!
Dear Jennie,
I love the comment you posted from Dr. Klimas about the medical profession giving us PTSD. It is such a good description (without me aiming to trivialize PTSD).
It was a beautiful description of the ridiculousness of trying to be a standardized patient while you are non-standard – so you’re acting all the time. You made me realize how much I pretent/act/try to separate out things doctors think they can do something about from the ones I know they are useless at – so as to get at least some appropriate medical care.
Ignoring new symptoms, blaming it all on the CFS, could be fatal.
I just got out of a two week period which took cardiologists trying to figure out chest pain 9 hospital days, a stress test, three catheterizations (the second with one stent and no solution, the third finally putting in two more stents and an angioplasty – and finding the 95% blockage). Between the drugs they gave me (which have taken almost another month for me to get off and get rid of the side effects), and the constant stress of new people, lack of control, CFS brain fog made worse, and hugely increased pain, I had come to the same description of the process: they caused it – so I am very lucky it wasn’t even worse. (details on my blog)
It was surreal, and still is: the final side effect is a profound lassitude with inability to wake up in the mornings and get my eyes open, and no thinking that I can use to write fiction (which is what I do) during the day.
I realized why I hadn’t identified this as a side effect: it’s the only one that hasn’t hurt.
I think that because we have limited ways of staying ‘fit’ with CFS, we are at LARGER risk of things such as what just happened to me, clogged arteries, and we have much SMALLER ability to deal with it. Not a good combination.
Thanks for writing about your experience being the ‘standardized patient.’ It’s one I’m not likely to get, and sounded fascinating. I’m sorry it costs you so much afterward, and I understand the impulse to get out of the house and do SOMETHING, ANYTHING so you don’t go stir-crazy.
Alicia, I hope you feel better soon! It sounds pretty scary.
I completely missed that this was JOE’s experience. Sorry! Brain fog is heavy this morning, I think due to the one med I can’t give up because the stents are then at larger risk of closing up, Effient.
Fantastic piece. Thank you for writing it. I can relate, and I’m sure many other PWCs can, too.
This is a beautiful piece, Joe, even as it’s heartbreaking. Thank you for writing it.
Leslie Jamison wrote about her experience in this line of work in her book The Empathy Exams, one of the best books I read last year. She weaves the subject of empathy into essays on widely divergent topics, including the Barkley Marathon (a treacherous back-country ultra race created in homage to a prison break) and attending a conference for people who suffer from Morgellons disease (without condescension). While we hope that others will find more empathy for us, we can really only affect our own empathy. This book fosters that kind of introspection, more philosophically provocative than self-help how-to. If you were on the academic side before getting sick, it’s a rewarding read.
Publisher’s Weekly summarizes: “Beginning with her experience as a medical actor who was paid to act out symptoms for medical students to diagnose, Leslie Jamison’s visceral and revealing essays ask essential questions about our basic understanding of others: How should we care about each other? How can we feel another’s pain, especially when pain can be assumed, distorted, or performed? Is empathy a tool by which to test or even grade each other? By confronting pain—real and imagined, her own and others’—Jamison uncovers a personal and cultural urgency to feel. She draws from her own experiences of illness and bodily injury to engage in an exploration that extends far beyond her life, spanning wide-ranging territory—from poverty tourism to phantom diseases, street violence to reality television, illness to incarceration—in its search for a kind of sight shaped by humility and grace.”
This book is in my reading queue!
I hope you like it as much as I did. But let me/us know either way. I’m reading Rebecca Solnit’s Hope in the Dark: Untold Histories, Wild Possibilities, which the blog Brainpickings has covered a few times in the last couple of months. It’s forthrightly political in a left-leaning way, and yet personal. This intro to Solnit’s book from the blog editor could be talking about how any of us think of ourselves in relationship to our illness
“The stories we tell ourselves about our public past shape how we interpret and respond to and show up for the present. The stories we tell ourselves about our private pasts shape how we come to see our personhood and who we ultimately become. The thin line between agency in victimhood is drawn in how we tell those stories.
The language in which we tell ourselves these stories matters tremendously, too, and no writer has weighed the complexities of sustaining hope in our times of readily available despair more thoughtfully and beautifully, nor with greater nuance, than Rebecca Solnit does in Hope in the Dark: Untold Histories, Wild Possibilities.”
Because this book discusses politics, read in smaller bites and with caution if you’re feeling reactive about the things in the world that amp up legitimate fears. Read it and yourself like an archaeologist, pondering the minutiae of your responses to it and then the sense of “Hope in the Dark” is more possible.
Joe: Excellent! This should be submitted to other outlets, like the New Yorker or the New York Times, under their new disabled personal essays section. (https://www.nytimes.com/column/disability) Just find out if they accept previously published pieces first. Or, better yet, just re-write this and shift some things around and then submit it anew to the above mentioned outlets.
I agree with Rivka. Ever since his duck days Joe Landson has a talent for humor–in a situation that is extraordinarily both serious and absurdly wrong.
And how many things do we honestly have left to make this experience tolerable? Humor, especially humor in absurdity, always asserts itself. It’s great to find essays that can highlight the absurdity and make us laugh.
They say laughter is the “best medicine” and for us… thanks to NIH, CDC inaction… it is one of the only ones!
Definitely kafkaesque.
Thanks, Joe, for your wonderful way with words (even though the reality of it all just plain sucks). I guess our biggest hope is to one day be lucky enough to actually be considered a “standard” patient again…sounds heavenly, doesn’t it?
You are an amazing autobiographical storyteller. I hope to one day help you become standard ?
I think Joe gives the medical profession an easy out when he says it’s not the doctors’ fault that they’re ignorant. It’s true that they don’t get much good information about ME/CFS. But I learned early on in my 30+ years with this disease that although doctors like to call themselves scientists, medicine isn’t a scientific profession; it’s an authoritarian one. Doctors believe what they’ve been taught to believe, even when that requires them to ignore what they observe–and definitely when it requires them to disbelieve what patients tell them. All too many of them have been taught to believe that (a) ME/CFS isn’t a real disease, (b) if we have a real illness, it’s a psychological one, and (c), there’s nothing they can do for us except feed us anti-depressants–and ignore the fact that many of them not only don’t help us but actually make us worse–and keep telling us we’re not really sick.
So when I hear some doctor describing his “scientific” approach to treating his or her patients, I’d fall down laughing, except that I don’t have the energy to pick myself up afterward.
Linda thanks,
I did give doctors a bit of an easy out, on the theory that we may need them later, when they finally get a clue.
Otherwise I agree, doctors are usually about medical authority, rather than about medical science.
Shared 😉