 In April 2019, NIH finally published their funding numbers for ME/CFS research in 2018. That means it is time for another fact-check and correction!
In April 2019, NIH finally published their funding numbers for ME/CFS research in 2018. That means it is time for another fact-check and correction!
Update October 16, 2019: as explained below, I received more accurate numbers from NIH and have updated this post to reflect that. For ease of reading, I changed numbers throughout this post as warranted without striking through every previous number. I have also updated the graph, and my original post about 2018 funding.
For the second year in a row, NIH has significantly overstated its investment. For 2018, NIH claims it spent 9% (almost $1.3 million) more than it actually spent. NIH also claims that funding fell by 4.5%, when the truth is that our funding fell by almost twice as much. In a disease like ME/CFS, this has serious consequences because the funding number is at the center of so much policy debate and advocacy efforts.
How Much Was Spent in 2018?
On the Categorical Spending Chart, NIH states that it spent $14 million on ME/CFS in 2018. The chart links to the list of projects and grants included in that number. Here is how it breaks down:
- Extramural grants: $4,663,553
- Collaborative Research Centers: $6,959,487
- Intramural projects: $2,417,815
This comes to a total of $14,040,855, which NIH rounds down to $14 million. But there’s a problem, and it’s the same problem I found in 2017. The intramural number is not limited to money spent on ME/CFS.
The Intramural Problem
NIH lists three intramural projects in 2018:
- Dr. Avindra Nath’s Clinical Care Center study: $750,000
- Dr. Leorey Saligan, “Investigating Correlates and Therapeutics of Fatigue”: $172,552
- Dr. David Goldstein, “Biomarkers of Catecholaminergic Neurodegeneration”: $1,495,263
*record scratch* $1.5 million to Dr. Goldstein for biomarkers? For real?
Actually no, that number is not for real, at least not as far as ME/CFS is concerned. Dr. Goldstein’s project page lists a number of different projects, most of which are related to Parkinson’s Disease. The connection to ME/CFS is the fifth item listed under Collaborations:
e) Clinical catecholamine neurochemistry in chronic fatigue syndrome: We are collaborating in an intramural study of chronic fatigue syndrome (NIH Clinical Protocol 16-N-0058, Myalgic Encephalomyelitis/ Chronic Fatigue Syndrome, PI Avindra Nath) by conducting screening autonomic function testing and provocative tilt table testing and assaying plasma and cerebrospinal fluid levels of catechols.
No specific amount of funding is listed for any of the subprojects on Dr. Goldstein’s intramural study. I ran into the same problem last year. In 2017, NIH included the full cost of the Human Energy and Body Weight Regulation Core in its ME/CFS spending, despite the fact that the funding was actually spent on twenty-six different clinical protocols. When I asked NIH how much of the funding could fairly be allocated to Dr. Nath’s study, the NIDDK Office of Communication said there was no such breakdown available. I had to guesstimate how much funding to include in 2017, and originally, I had to do the same for 2018 as well.
I divided the Goldstein funding among all the listed subprojects and collaborations, and arrived at a 2.5% share to the ME/CFS study. Is that fair or correct? No idea!!! The lack of precision in NIH’s accounting (at least publicly) means we have to guess. One thing I do know for sure: NIH should not claim the entire $1.5 million from Goldstein’s work in the ME/CFS category. It artificially inflates the funding number by a significant amount.
In June 2019, I asked NIH for the actual amount that Dr. Goldstein spent on his ME/CFS project. In September 2019, Dr. Vicky Whittemore informed me that Dr. Goldstein’s laboratory:
spends about 15% of his resources on ME/CFS research, including their testing equipment in the Patient Observation Room, Research Nurse, Clinical Research Nurse Practitioner, catechol assay personnel and systems, reagents and disposables, computer software and hardware, and his time and effort. This is all factored into the overall budget his lab receives and his lab does not receive specific funds that are designated to be spent on ME/CFS research. The budgets for the intramural labs are provided to the lab overall and they don’t allocate or budget for specific research projects – they just do the research.
Accordingly, I applied 15% of Dr. Goldstein’s budget ($224,289) to the ME/CFS total. Back in October, I calculated that NIH spent $11,623,040 in 2018. With the addition of the Nath, Saligan, and Goldstein intramural funding, I now calculate that NIH actually spent $12,769,881 in 2018.*
How Big Is The Difference?
NIH’s failure to accurately report the intramural funding number results in a significant overstatement of the ME/CFS investment for both 2017 and 2018.
| NIH Calculation | My Calculation | NIH Overestimate | |
|---|---|---|---|
| FY 2017 | $14,725,728 | $13,967,704 | 5% more than spent |
| FY 2018 | $14,040,855 | $12,769,881 | 9% more than spent |
In case the table is unclear, NIH overestimated its ME/CFS spending in 2018 by 9%, or almost $1.3 million. The overestimate is due to NIH’s failure to assign the correct amount of intramural funding to the ME/CFS total.
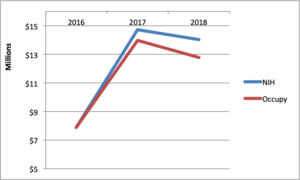
The inflation of the funding number also affects the calculation of changes in funding from year to year. Using NIH’s numbers, funding decreased by 4.6% from 2017 to 2018. But using the actual amount spent on ME/CFS, funding decreased by 8.5% in 2018. Here’s a graph of NIH’s calculation compared to mine for 2016 through 2018:
When NIH reports inaccurate numbers on its Categorical Spending Chart, those numbers are relied upon by Congress, journalists and advocates, even though the numbers are actually wrong.
The September 2019 Report of the NANDS Council Working Group For ME/CFS Research is a prime example. That report uses NIH’s inflated funding numbers in multiple places, including Figure 1 on page 7. Because this is an official report, the inaccurate numbers will be enshrined in all subsequent discussions. In a research area like ME/CFS, where the annual investment is so incredibly low, relying a number that is off by more than $1 million is a big deal. That $1.3 million is almost enough to fund another Research Center for a year. It makes it look like NIH is doing substantially more than it actually is.
Reporting that funding declined by 4.5%–when it is actually 8.5%–is significant. It obscures the truth and minimizes the very serious funding problem in ME/CFS research. Counting money towards ME/CFS that was not actually spent that way, even if it is due to a sloppy accounting policy and not malfeasance, is misleading. This is true for every research category, but the effect is much stronger for diseases like ME/CFS that are already subsisting on tiny crumbs from the NIH budget.
This is yet another way that the burden of accuracy and attention to detail is shifted to our disease community that is already carrying so much. Why did I have to invest hours of my time over several weeks to ferret out the correct number and pass that information on to you? Why should I have to make my self sicker and do NIH’s accounting job?
Because it has to be done. We need the accurate numbers, and we need to use them everywhere. Use them in talking to Congress, in asking questions of NIH, in participating in discussions like the NANDS Working Group, in speaking publicly about the ME public health crisis, and in writing about it.
I believe my work has shown–over many years–that regardless of the intentions of individuals at NIH and other agencies, we cannot assume that the agencies will do the right thing and report the right thing to us. We have to do this fact-finding work in order to hold them accountable.
If our goal is to secure more research funding in order to identify treatments for patients, then use the correct information. NIH spent $12.8 million on ME/CFS in 2018, not the $14 million that they claim. Funding was down 8.5% in 2018, and we slide backwards down the funding ramp that Dr. Francis Collins had promised us.
Use the correct information. Require NIH to use the correct information, too. And trumpet the truth: ME/CFS funding at NIH fell by 8.5% in 2018.
*I’ve corrected that earlier post with these new numbers.

Holding out for better news in 2019.. Thanks Jennie for such huge efforts in getting accurate info. As you say, it will be useful for the working group.
I am sorry for the toll it takes on you to show the defects in NIH’s accounting – though I greatly appreciate that you do this for us!
NIH – Falling funding is so unfair for a disease that is already woefully underfunded. This cannot go on. We deserve appropriate funding and accurate accounting by NIH.
We are so lucky to have you do this work. I’m so sorry it takes such a toll on your health.
Truly, what is wrong with our National Institutes of Health?
Jenny , I solute you for the incredible job you doing , we are lucky to have you . Sometimes it feels like a war without end . I keep asking myself , is it lack of empathy , corruption or what ????? Can’t come up with an answer , hope somebody will . Thank you again and again . Wish you health , keep fighting .
If you (and possibly a few others like you involved in getting the grants) don’t do this, the NIH and its top executives get away with putting out the same old fake news: say what you want, as no one care or checks.
And if taxed, will probably blame an underling.
I don’t know how you have the stomach for it, you and David Tuller, but I’m glad you do. And I thank you for spending your precious energy on this garbage we are offered as ‘food.’
Jennie,
You are one of our sheroes with your analysis! Thank you for once again highlighting important information.
JENNIE, YOU ARE MAGNIFICENT!!!
This is not heroic, but super-heroic work on the level of Alem Mattees and Tom Kindlon. I don’t know where we would be without you. Praying you feel the sacrifice is worth it. Rest now and let us trumpet your achievement. NIH lies show their shame: the edifice the BPS lobby have shored up for so long is slowly crumbling. Take heart.
Much love and many thanks xxx
Goodness, I’m blushing! Thank you, Sam, and everyone.
You are amazing!!???
So now Whittemore says the NIH doesn’t have any extra money?
(expletives deleted)
Hi Jennie,
Thanks for doing all this painstaking work. I had hoped that one of our national advocacy organizations would take this work on as a way of measuring the efficacy of their efforts. Sadly none of them seem interested. The graph in Cort Johnson’s article (https://www.healthrising.org/blog/2019/02/16/lie-nih-accelerating_research-slogan-me-cfs/) displaying NIH CFS/ME funding as a percentage of it’s overall budget puts the reality of our situation in stark terms – so far the NIH is only capable of episodic funding bursts that do not endure. The NIH seems unwilling to make a sustained effort to increase ME/CFS research funding levels.
The question is why – what changes the behavior of the NIH? Is there some other chronic illness similar in nature to ME/CFS that the NIH ramped up research for in the past? I don’t know that AID’s is the best example of an illness to consider because healthy people could relate to it as a terminal acute illness not a lingering chronic one.
I think that there are important comparisons to AIDS to be made. This excerpt by Kenneth J. Friedman, from https://www.frontiersin.org/articles/10.3389/fped.2019.00131/full is an example:
“Despite HIV/AIDS currently being considered a manageable disease, the proposed U.S. HIV/AIDS budget for 2018 was $32 billion of which 85 % ($20.7 billion) was for domestic care and treatment programs, 9% ($3.1 billion) for domestic care and housing assistance, 7 % ($2.2 billion) for domestic research, and 2 % ($0.7 billion) for domestic prevention (52). There are no domestic care, treatment, prevention, or housing programs for ME/CFS patients. For ME/CFS, a disease estimated to have more than double the number of patients, and with a quality of life judged to be as or more diminished than that of HIV/AIDS, the disparity in patient care and patient benefits is unsettling.”
Dr. Friedman also says, “AIDS patients were identified in 1981 and the virus causing AIDS was identified in 1984 (79).” I got sick in 1983, like so many others who got sick in the 1980s, but we got cast aside and remain cast aside with the addition of decade’s worth of misinformation, stigmatization and discrimination. Cort tweeted https://twitter.com/CortJohnson/status/1114281540333318144, “#MECFSatNIH19 – Maureen Hanson – talks about upsurge in cases 35 years ago….something happened.” I agree, something happened and they can’t just keep sweeping it and us under the rug like it didn’t happen and like we aren’t really out here in desperate need of help and justice!
There is so much that the NIH could do to stop this discrimination if they had the will to do it. This is also from Dr. Friedman’s article:
“Some of the professional scientists who have pursued ME/CFS have jeopardized their careers and livelihood (31). Medical school clinicians have been told to stop seeing ME/CFS patients because they require too much of a clinician’s time, and, if they do not stop, they will need to work elsewhere. Researchers have been told that ME/CFS research will not be considered for their promotions, and if they are not promoted, they will need to leave the institution. Medical educators have been told that ME/CFS educational activities are not, “professional,” and those activities are banned from the workplace. While the NIH State of Knowledge ME/CFS Workshop, held in 2011, exposed and documented these problems (31), there has been no documentation of NIH objecting to any of these practices. NIH could withhold or limit funding to institutions which discourage or do not permit medical research and patient care for diseases that are of importance to the NIH. Not even the American Association of University Professors (AAUP), which claims academic freedom as its core mission (32), has objected to academic, institutional bans on ME/CFS research, clinical care, and educational activities.”
If the NIH withheld or limited funding, institutions would very quickly get the message that ME/CFS is a disease to take seriously and that would also generate more grant applications.
Hi Laurie,
I agree that it is useful to compare the governments response to AIDS with their [non] response to ME/CFS as a way of illustrating the iniquities of the situation. However the political dynamics in each case are different enough to make me think that the ME/CFS community should consider other historical examples where a disease that was being ignored finally evoked a response from the government commensurate with the suffering it caused. With AIDS the attitudes of the lay public could be enlisted to generate political pressure for an adequate government response. I think it will be much more difficult to enlist the lay public on our side – we have a weird illness and more to the point most of the authoritative medical organizations have a hostile or indifferent attitude to us. It was hard for physicians to claim that AIDS was not a serious problem when it was A: a communicable illness and B: people died from it in easily observable ways in a relatively short period of time. The ME/CFS community is thus faced with 2 obstacles – the ignorance of the lay public and the active hostility from sections of the medical establishment. I have read that MS sufferers were in a similar situation in the past – chronic disabling illness like MS are a probably better comparison for ME/CFS than AIDS in terms of the political dynamics of government / medical response. If I have some energy I may look into the history of MS and how it became a “politically correct” illness within the medical community.
This article looked interesting: https://mpkb.org/home/alternate/psychosomatic
Her e is a link to a very interesting article discussing the history of CFS: https://www.ncbi.nlm.nih.gov/pubmed/16085995.
ABSTRACT: In 1868, Jean-Martin Charcot identified multiple sclerosis (MS) as a distinct nosological entity. By 1870,American neurologists became aware of the new disease and began to diagnose cases in the United States. For the next 50 years, however, American physicians thought it was a rare condition. From 1920 to 1950, this perception changed dramatically; by 1950, neurologists considered it among the most common neurological diseases in America. The increasing prevalence of MS between 1920 and 1950 can largely be explained as an effect of an increase in the number of trained neurologists, urbanization, a changed ecology of disease, and altered concepts of gender and disease. Physicians recognized MS more frequently because over time there were more neurologists who had the skills necessary to make the difficult diagnosis, and because patients were more likely to be seen by a trained neurologist. Significant numbers of patients with MS had been misdiagnosed with other diseases such as hysteria and neurosyphilis; over time, they were increasingly diagnosed correctly.
WE DO NOT HAVE ACCURATE AND RELIABLE STATISTICS for the prevalence of multiple sclerosis (MS) in the United States until the late 1940s, but the literature clearly expresses a changing perception of the frequency of this disease (Kurland 1994). Jean-Martin Charcot, working in France, identified MS as a distinct nosological entity in 1868. More than two decades later, in 1892, Charles Dana reflected the standard view among neurologists when he wrote that “in America the disease is, in the writer’s experience, rare.” Analysis of the diagnoses reported in the New York Hospital Annual Reports from 1883 to 1906 shows that physicians diagnosed MS only 10 times for inpatients; between 1892 and 1906, they diagnosed MS five times at the outpatient House of Relief. In the early 20th century, some neurologists began to question the idea that MS was rare in America, because they recognized how difficult it was to diagnose the condition (Dercum and Gordon 1905; Putnam 1903). Nevertheless, the general perception remained through the first decade of the century that MS was rare in America (Crafts 1917).
These statistics and continuing suspicions about misdiagnosed cases led, during the 1920s, to assertions by neurologists that MS was an infrequent disease, but one that was increasing slowly (Taylor 1922). Nonetheless, the diagnosis of MS remained uncommon. In 1928, two physicians reported that “at the Philadelphia General Hospital from 1920 to 1926 inclusive there were studied 6,974 cases in the neurological wards and the diagnosis of multiple sclerosis was made twenty-four times (0.33 percent) (Potts and Drake 1928).
By the early 1930s, many neurologists’ perception of the frequency of MS had begun to change more dramatically (De Nicola 1933; Odell 1931). In 1931, Sidney D.Wilgus and Egbert W. Felix wrote that “Multiple Sclerosis is a common disease, and hence the importance of recognizing its early symptoms is worth emphasizing.”This shift in perception continued in the early and middle 1940s. Tracy Putnam (1943) wrote: “it is clear that in this locality [New York City] at least,multiple sclerosis is by no means a rare disease.” By the late 1940s and early 1950s, some American neurologists saw MS as among the most common disease of the central nervous system. In 1948, one group of neurologists estimated that there were 50,000 to 90,000 MS patients in the United States (Merritt,Wortis, andWoltman 1950). In that same year,Charles C. Limburg (1950) estimated that there might be as many as 150,000 patients with MS. University of Wisconsin Professor Hans Reese (1949) declared that “among the diseases of the central nervous system, multiple sclerosis ranks today almost as the most frequent illness.” What explains the changed perception of MS as a rare disease as late as 1920 to a common one by 1950?
Hi, Marc. You may be interested in this history of MS from the National Multiple Sclerosis Society https://www.nationalmssociety.org/NationalMSSociety/media/MSNationalFiles/Brochures/Brochure-History-of-Multiple-Sclerosis.pdf.
I’m just going to post here about the 1990s. While we were being labeled with Yuppie Flu, this is what was going on in MS research:
1990s: Decade of The Brain
As the final decade of the 20th century approached, the Congress of the United States made a special effort to accelerate medical research. Recognizing the paramount importance of neurological disease, they designated the 1990s as the “Decade of the Brain” and purposefully funneled funds, time, and talent into the treatment of illnesses that affect the nervous system. MS benefited enormously from these efforts, and an explosion of treatment trials occurred during this period.